

The Role of Skin Health in Holistic Living
Discover how skin health mirrors overall wellbeing in holistic living, including the impact of stress, lifestyle habits, and internal balance.


Common Bone And Joint Problems Treated By Orthopedic Specialists
Learn about common bone and joint conditions treated by orthopedic specialists, including knee pain, arthritis, back pain, and sports-related injuries.


Should Mental Health Therapists Handle Billing In-House or Outsource?
Explore whether in-house or outsourced mental health billing is better for reducing denials, improving revenue, and easing admin stress.


The Impact of Recognition on Wellness Team Morale and Motivation
Boost team morale by implementing effective staff recognition strategies in wellness businesses for better employee engagement.


What Causes Vaginal Irritation Without Infection?
Learn common non-infectious causes of vulvar irritation, from pH shifts and friction to hormones, stress, and product sensitivity.

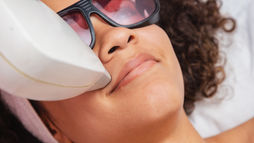
Safe Aesthetic Care: Protecting Your Skin Prior to and Post Treatment
Discover how aesthetic care can enhance your skin's texture and brightness while prioritising safety and professional evaluation.

The Quiet Power of Southeast Asian Botanical Remedies in Modern Wellness
Explore how Southeast Asian botanical remedies support modern wellness through mindful rituals, herbal traditions, and recovery.


How Families Can Support a Loved One Through Mental Health & Addiction Recovery: A Compassionate Guide
Learn how families can support addiction recovery with healthy boundaries, compassion, and emotional support.


5 PMDD Self CareTips That Can Help You Protect Your Energy and Emotions
Explore effective pmdd self-care strategies to protect emotional stability and energy throughout the menstrual cycle.






